CryoStor® CS10
Animal component-free, defined cryopreservation medium with 10% DMSO
概要
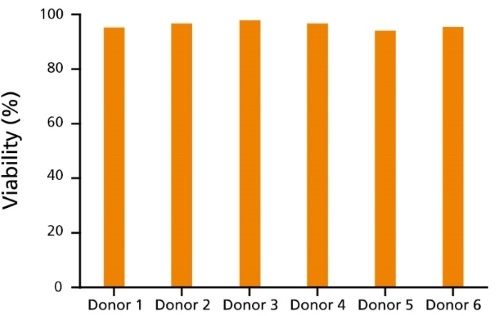
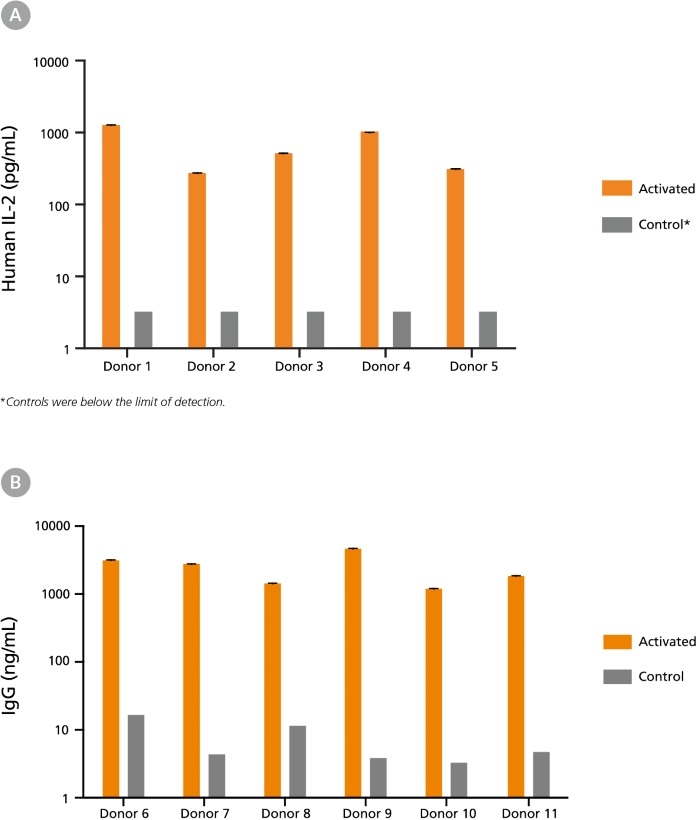
CryoStor® CS10 is a uniquely formulated serum-free, animal component-free, and defined cryopreservation medium containing 10% dimethyl sulfoxide (DMSO). Designed to preserve cells in low temperature environments (-80°C to -196°C), CryoStor® CS10 provides a safe, protective environment for cells and tissues during the freezing and thawing processes and during storage. CryoStor® CS10 is recommended for the cryopreservation of hepatocytes, tissue samples, human peripheral blood, CHO cells, myeloma cell lines, hybridomas, human mesenchymal stem cells, human embryonic and human induced pluripotent stem cells (ES cells and iPS cells) and other extremely sensitive cell types. CryoStor® CS10 is cGMP-manufactured with USP grade components.
• Ready-to-use
• Serum-free and protein-free
• Animal component-free
• cGMP manufactured with USP grade/highest-quality components
• FDA master file
• Sterility, endotoxin, and cell-based quality control testing
• 10% dimethyl sulfoxide (DMSO)
• Other ingredients
B Cells, CHO Cells, Hematopoietic Stem and Progenitor Cells, Hybridomas, Intestinal Cells, Macrophages, Mesenchymal Stem and Progenitor Cells, Monocytes, Myeloma, NK Cells, Other, Pluripotent Stem Cells, T Cells
Human, Mouse, Rat, Non-Human Primate, Other
Cord Blood Banking, Epithelial Cell Biology, Immunology, Stem Cell Biology
数据及文献
Publications (61)
Nature immunology 2019 The immune cell landscape in kidneys of patients with lupus nephritis. A. Arazi et al.
Abstract
Lupus nephritis is a potentially fatal autoimmune disease for which the current treatment is ineffective and often toxic. To develop mechanistic hypotheses of disease, we analyzed kidney samples from patients with lupus nephritis and from healthy control subjects using single-cell RNA sequencing. Our analysis revealed 21 subsets of leukocytes active in disease, including multiple populations of myeloid cells, T cells, natural killer cells and B cells that demonstrated both pro-inflammatory responses and inflammation-resolving responses. We found evidence of local activation of B cells correlated with an age-associated B-cell signature and evidence of progressive stages of monocyte differentiation within the kidney. A clear interferon response was observed in most cells. Two chemokine receptors, CXCR4 and CX3CR1, were broadly expressed, implying a potentially central role in cell trafficking. Gene expression of immune cells in urine and kidney was highly correlated, which would suggest that urine might serve as a surrogate for kidney biopsies.
Cell stem cell 2018 MAY Super-Obese Patient-Derived iPSC Hypothalamic Neurons Exhibit Obesogenic Signatures and Hormone Responses.
U. Rajamani et al.
Abstract
The hypothalamus contains neurons that integrate hunger and satiety endocrine signals from the periphery and are implicated in the pathophysiology of obesity. The limited availability of human hypothalamic neurons hampers our understanding of obesity disease mechanisms. To address this, we generated human induced pluripotent stem cells (hiPSCs) from multiple normal body mass index (BMI; BMI ≤ 25) subjects and super-obese (OBS) donors (BMI ≥ 50) with polygenic coding variants in obesity-associated genes. We developed a method to reliably differentiate hiPSCs into hypothalamic-like neurons (iHTNs) capable of secreting orexigenic and anorexigenic neuropeptides. Transcriptomic profiling revealed that, although iHTNs maintain a fetal identity, they respond appropriately to metabolic hormones ghrelin and leptin. Notably, OBS iHTNs retained disease signatures and phenotypes of high BMI, exhibiting dysregulated respiratory function, ghrelin-leptin signaling, axonal guidance, glutamate receptors, and endoplasmic reticulum (ER) stress pathways. Thus, human iHTNs provide a powerful platform to study obesity and gene-environment interactions.
Stem cell reports
2018
MAY
Inflammatory Responses and Barrier Function of Endothelial Cells Derived from Human Induced Pluripotent Stem Cells.
O. V. Halaidych et al.
Abstract
Several studies have reported endothelial cell (EC) derivation from human induced pluripotent stem cells (hiPSCs). However, few have explored their functional properties in depth with respect to line-to-line and batch-to-batch variability and how they relate to primary ECs. We therefore carried out accurate characterization of hiPSC-derived ECs (hiPSC-ECs) from multiple (non-integrating) hiPSC lines and compared them with primary ECs in various functional assays, which included barrier function using real-time impedance spectroscopy with an integrated assay of electric wound healing, endothelia-leukocyte interaction under physiological flow to mimic inflammation and angiogenic responses in in vitro and in vivo assays. Overall, we found many similarities but also some important differences between hiPSC-derived and primary ECs. Assessment of vasculogenic responses in vivo showed little difference between primary ECs and hiPSC-ECs with regard to functional blood vessel formation, which may be important in future regenerative medicine applications requiring vascularization.
The Journal of clinical investigation
2018
JUN
Dose intensification of TRAIL-inducing ONC201 inhibits metastasis and promotes intratumoral NK cell recruitment.
J. Wagner et al.
Abstract
ONC201 is a first-in-class, orally active antitumor agent that upregulates cytotoxic TRAIL pathway signaling in cancer cells. ONC201 has demonstrated safety and preliminary efficacy in a first-in-human trial in which patients were dosed every 3 weeks. We hypothesized that dose intensification of ONC201 may impact antitumor efficacy. We discovered that ONC201 exerts dose- and schedule-dependent effects on tumor progression and cell death signaling in vivo. With dose intensification, we note a potent anti-metastasis effect and inhibition of cancer cell migration and invasion. Our preclinical results prompted a change in ONC201 dosing in all open clinical trials. We observed accumulation of activated NK+ and CD3+ cells within ONC201-treated tumors and that NK cell depletion inhibits ONC201 efficacy in vivo, including against TRAIL/ONC201-resistant Bax-/- tumors. Immunocompetent NCR1-GFP mice, in which NK cells express GFP, demonstrated GFP+ NK cell infiltration of syngeneic MC38 colorectal tumors. Activation of primary human NK cells and increased degranulation occurred in response to ONC201. Coculture experiments identified a role for TRAIL in human NK-mediated antitumor cytotoxicity. Preclinical results indicate the potential utility for ONC201 plus anti-PD-1 therapy. We observed an increase in activated TRAIL-secreting NK cells in the peripheral blood of patients after ONC201 treatment. The results offer what we believe to be a unique pathway of immune stimulation for cancer therapy.
Arthritis research & therapy
2018
JUL
Methods for high-dimensonal analysis of cells dissociated from cyropreserved synovial tissue.
L. T. Donlin et al.
Abstract
BACKGROUND Detailed molecular analyses of cells from rheumatoid arthritis (RA) synovium hold promise in identifying cellular phenotypes that drive tissue pathology and joint damage. The Accelerating Medicines Partnership RA/SLE Network aims to deconstruct autoimmune pathology by examining cells within target tissues through multiple high-dimensional assays. Robust standardized protocols need to be developed before cellular phenotypes at a single cell level can be effectively compared across patient samples. METHODS Multiple clinical sites collected cryopreserved synovial tissue fragments from arthroplasty and synovial biopsy in a 10{\%} DMSO solution. Mechanical and enzymatic dissociation parameters were optimized for viable cell extraction and surface protein preservation for cell sorting and mass cytometry, as well as for reproducibility in RNA sequencing (RNA-seq). Cryopreserved synovial samples were collectively analyzed at a central processing site by a custom-designed and validated 35-marker mass cytometry panel. In parallel, each sample was flow sorted into fibroblast, T-cell, B-cell, and macrophage suspensions for bulk population RNA-seq and plate-based single-cell CEL-Seq2 RNA-seq. RESULTS Upon dissociation, cryopreserved synovial tissue fragments yielded a high frequency of viable cells, comparable to samples undergoing immediate processing. Optimization of synovial tissue dissociation across six clinical collection sites with {\~{}} 30 arthroplasty and {\~{}} 20 biopsy samples yielded a consensus digestion protocol using 100 mu$g/ml of Liberase™ TL enzyme preparation. This protocol yielded immune and stromal cell lineages with preserved surface markers and minimized variability across replicate RNA-seq transcriptomes. Mass cytometry analysis of cells from cryopreserved synovium distinguished diverse fibroblast phenotypes, distinct populations of memory B cells and antibody-secreting cells, and multiple CD4+ and CD8+ T-cell activation states. Bulk RNA-seq of sorted cell populations demonstrated robust separation of synovial lymphocytes, fibroblasts, and macrophages. Single-cell RNA-seq produced transcriptomes of over 1000 genes/cell, including transcripts encoding characteristic lineage markers identified. CONCLUSIONS We have established a robust protocol to acquire viable cells from cryopreserved synovial tissue with intact transcriptomes and cell surface phenotypes. A centralized pipeline to generate multiple high-dimensional analyses of synovial tissue samples collected across a collaborative network was developed. Integrated analysis of such datasets from large patient cohorts may help define molecular heterogeneity within RA pathology and identify new therapeutic targets and biomarkers.
Oncotarget
2018
JAN
CD34- human placenta-derived mesenchymal stem cells protect against heat stroke mortality in rats.
W. Lin et al.
Abstract
CD34 is a transmembrane phosphoglycoprotein used to selectively enrich bone marrow in hematopoietic stem cells for transplantation. Treating rats with CD34+ cells derived from human umbilical cord blood before or after heat stroke has been shown to promote survival. We investigated whether CD34- human placenta-derived stem cells (PDMSCs) could improve survival following heat stroke in rats. Rats were subjected to heat stress (42°C for 98 min) to induce heat stroke. Intravenous administration of PDMSCs 1 day before or immediately after the onset of heat stroke improved survival by 60{\%} and 20{\%}, respectively. Pre-treatment with CD34- PDMSCs protected against heat stroke injury more effectively than that treatment after injury. PDMSCs treatment attenuated cerebrovascular dysfunction, the inflammatory response, and lipid peroxidation. These data suggest human PDMSCs protect against heat stroke injury in rats. Moreover, these effects do not require the presence of CD34+ cells.